Peeling skin on the bottom of the feet is a surprisingly common issue, yet it can be both uncomfortable and concerning. Whether you’ve noticed flaky patches after a beach day, persistent scaling despite moisturizing, or sudden peeling with no clear cause, understanding the root of the problem is key to effective treatment. This condition can stem from something as simple as dry skin or as serious as an autoimmune disorder. Ignoring it—especially if you have diabetes or poor circulation—can lead to infections, ulcers, or more severe complications.
The causes range from environmental triggers like hot showers and tight shoes to medical conditions such as fungal infections, eczema, psoriasis, and even systemic diseases like diabetes or hypothyroidism. Some people experience seasonal peeling due to heat and sweat, while others may react to allergens in footwear or medications. The good news? Most causes are treatable once properly identified. In this guide, you’ll learn how to distinguish between common and serious causes, what symptoms to watch for, and when it’s time to see a doctor.
Dry Skin and Its Triggers
Dry skin, or xerosis, is the most frequent reason for peeling soles. The feet naturally produce less oil than other body parts, making them prone to moisture loss, especially under constant pressure and friction.
Why Feet Lose Moisture
Environmental and lifestyle factors strip the skin of its natural oils. Cold weather, low humidity, and indoor heating reduce moisture in the air. Long, hot showers or harsh soaps further damage the skin barrier. Aging also plays a role—sweat and sebum production decline over time, leaving skin drier and more fragile.
People who stand for long periods, wear non-breathable shoes, or don’t hydrate well are at higher risk. The result? Tight, rough, flaky skin, often with deep cracks—especially on the heels.
Signs It’s Just Dry Skin
- Flaking or scaling without redness or itching
- Mild discomfort or tightness
- Cracks that worsen in winter
- Improvement with regular moisturizing
If this sounds familiar, simple changes can help. But if peeling persists or worsens, another cause may be at play.
Athlete’s Foot: Fungal Infection Signs
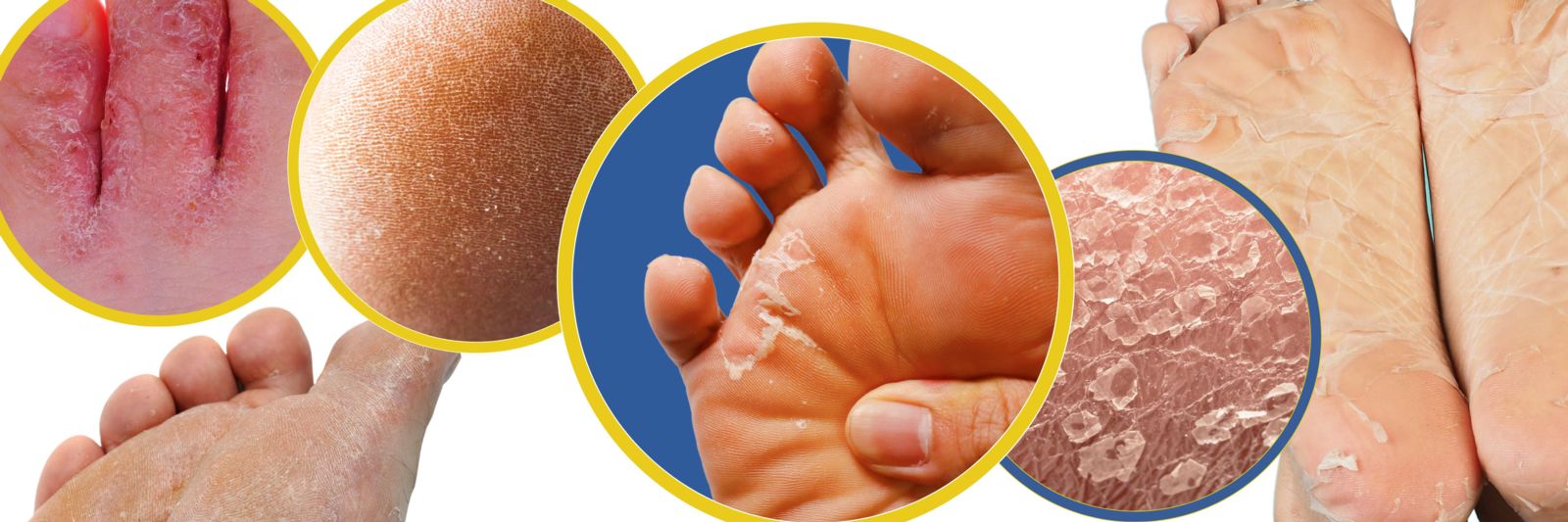
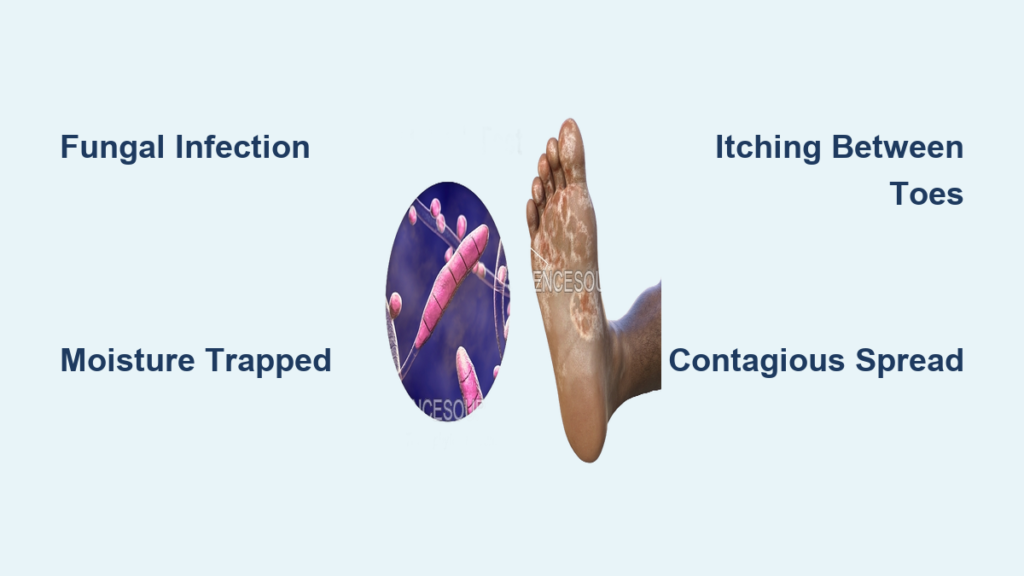
Athlete’s foot isn’t just for athletes. It’s a fungal infection that thrives in warm, damp environments—like sweaty shoes or public showers.
How Fungus Causes Peeling
Dermatophytes, especially Trichophyton rubrum, invade the outer layer of skin. They feed on keratin, breaking down the skin structure and causing it to flake, crack, and peel. The infection often starts between the toes but spreads to the soles.
You’re more likely to get it if you:
– Wear tight, synthetic shoes
– Sweat heavily (hyperhidrosis)
– Walk barefoot in gyms, pools, or locker rooms
– Share towels or footwear
Key Symptoms to Watch For
- Peeling with redness or itching
- Foul odor from feet or shoes
- Blisters or moist, white patches between toes
- Thick, discolored toenails (sign of onychomycosis)
Peeling without itching doesn’t rule out fungus—some cases are “silent” but still contagious.
How to Confirm and Treat It
A doctor can diagnose athlete’s foot by examining a skin scraping under a microscope (KOH test). Over-the-counter antifungals like terbinafine (Lamisil) or clotrimazole (Lotrimin) work well when applied twice daily to clean, dry skin.
Pro tip: Continue treatment for 2–4 weeks after symptoms disappear to prevent recurrence.
Excessive Sweating and Skin Breakdown
Hyperhidrosis—excessive sweating—can be just as damaging as dryness. Constant moisture softens the skin, leading to maceration and peeling.
Why Wet Skin Peels
When feet stay damp, the skin turns white, soggy, and fragile. This breakdown increases the risk of fungal and bacterial infections. Peeling is often widespread, affecting the entire sole.
Common triggers:
– Hot weather
– Stress
– Non-breathable shoes
– Hyperhidrosis (a medical condition)
Managing Overactive Sweat Glands
- Aluminum chloride (Drysol): A strong antiperspirant applied at night
- Glycopyrronium wipes: Reduce sweat production
- Iontophoresis: Uses water and mild electrical current to decrease sweating
- Botox injections: For severe cases; lasts 3–6 months
Wearing moisture-wicking socks and rotating shoes helps keep feet dry.
Eczema on the Soles: What to Know
Eczema isn’t just for elbows and knees—it can affect the feet too, especially in people with a history of allergies, asthma, or sensitive skin.
Triggers That Cause Flare-Ups
Foot eczema is often triggered by:
– Harsh soaps or detergents
– Fragranced lotions or foot sprays
– Wool or synthetic socks
– Stress or temperature changes
It may appear as dry, red, scaly patches on the soles, heels, or sides of the feet.
How It Differs from Other Causes
Unlike athlete’s foot, eczema often itches intensely. Unlike dry skin, it may blister or weep. It tends to be chronic, with flare-ups and remissions.
Effective Treatment Steps
- Moisturize daily with fragrance-free creams (ceramides, glycerin)
- Use topical steroids (e.g., hydrocortisone) during flares
- Avoid triggers—switch to hypoallergenic laundry detergent and shoe materials
- Try calcineurin inhibitors (tacrolimus) for sensitive areas
Antihistamines can help reduce nighttime itching.
Psoriasis: Autoimmune Skin Peeling
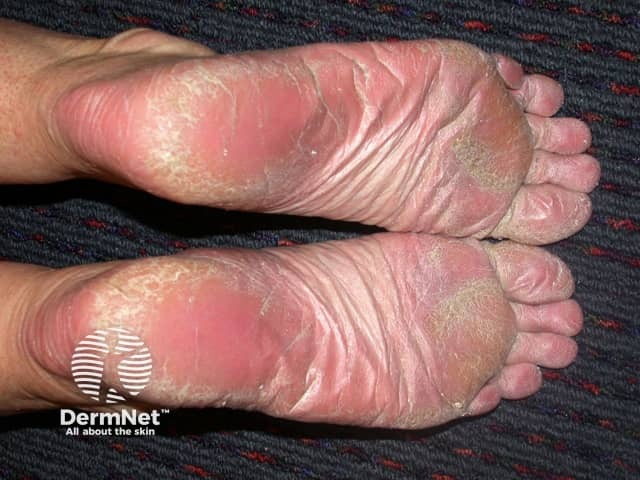
Psoriasis causes skin cells to grow too fast, building up into thick, scaly patches. When it affects the feet, it’s called palmoplantar psoriasis.
What Psoriasis Looks Like on Feet
- Red, well-defined patches with silvery scales
- Painful cracks that may bleed
- Burning or stinging sensation
- Often symmetrical (both feet affected)
It can be triggered by stress, injury (Koebner phenomenon), or cold weather.
Diagnosis and Treatment Options
A dermatologist may diagnose psoriasis by appearance or perform a biopsy. Treatment depends on severity:
- Topical steroids and vitamin D analogs (calcipotriene)
- Salicylic acid to remove thick scales
- Phototherapy (UVB) for widespread cases
- Systemic drugs (methotrexate, biologics) for severe disease
Psoriasis is chronic but manageable with consistent care.
Allergic Reactions from Shoes or Socks
Contact dermatitis occurs when skin reacts to an irritant or allergen—often from shoe materials, dyes, or sock fabrics.
Common Allergens in Footwear
- Rubber or latex in soles
- Leather tanning chemicals (chromates)
- Adhesives or dyes
- Synthetic fibers in socks
The reaction usually appears where the skin touches the material.
Symptoms and Diagnosis
- Red, itchy, peeling skin
- Blisters in severe cases
- Rash confined to contact areas
Patch testing by a dermatologist can identify the exact allergen.
How to Stop the Reaction
- Stop wearing the offending shoes or socks
- Use hypoallergenic alternatives (leather-free, cotton-lined)
- Apply topical steroids to reduce inflammation
- Moisturize to repair the skin barrier
Once the trigger is removed, symptoms usually improve in days.
Sunburn on the Soles: Overlooked Risk
Sunburn isn’t just for arms and shoulders. Lying on your stomach at the beach or walking barefoot on hot sand can expose your soles to UV rays.
Why Soles Get Burned
People often forget to apply sunscreen to the bottoms of their feet. UV exposure damages skin cells, leading to redness, pain, and peeling 3–7 days later.
Signs of a Sole Sunburn
- Red, tender skin
- Swelling or blistering (in severe cases)
- Peeling in large sheets days later
Immediate Care and Prevention
- Cool compresses or foot soaks
- Aloe vera gel for soothing
- Moisturizers and NSAIDs (ibuprofen) for pain
- Avoid further sun exposure
Prevention: Apply broad-spectrum SPF 30+ to soles when barefoot outdoors.
Recurring Peeling Without Itch: Keratolysis
Keratolysis exfoliativa (also called dyshidrosis lamellosa sicca) causes painless, recurring peeling on palms and soles—often in summer.
What It Feels and Looks Like
- Small, air-filled blisters that pop quickly
- Circular areas of peeling skin on forefoot or heels
- No redness, itching, or pain
- Episodes lasting days to weeks, then recurring
It’s more common in young adults and may be linked to heat, sweat, or frequent hand-washing.
How to Manage It
- Daily moisturizing with urea (10%) or lactic acid creams
- Avoid harsh soaps and irritants
- Wear breathable shoes
The condition is harmless and often resolves on its own.
Blisters and Friction-Related Peeling
Blisters from ill-fitting shoes can mimic peeling conditions when the top layer of skin tears off.
How Friction Causes Skin Loss
Repeated rubbing separates skin layers, filling the space with fluid. When the blister breaks, the dead skin peels away, leaving raw, sensitive tissue.
Proper Blister Care
- Leave intact if possible—the skin protects new tissue
- Cover with a blister pad or bandage
- If drained, use a sterilized needle and clean the area
- Apply antibiotic ointment if open
Prevent future blisters with well-fitted shoes and moisture-wicking socks.
Serious Medical Conditions Linked to Peeling
Persistent or widespread peeling can signal an underlying health issue—especially if other symptoms are present.
Diabetes and Foot Skin Changes
High blood sugar pulls fluid from tissues, drying the skin. Neuropathy reduces sweating, and poor circulation slows healing. Cracks and peeling can lead to ulcers and infections.
Critical for diabetics:
– Check feet daily
– Moisturize (but not between toes)
– Never walk barefoot
– See a podiatrist regularly
Hypothyroidism: Dry Skin from Low Metabolism
An underactive thyroid slows bodily functions, including sweat production. Skin becomes dry, thin, and flaky—often on the feet and legs.
Diagnosis: Blood test (TSH, T3, T4)
Treatment: Levothyroxine replacement
Venous Stasis Dermatitis
Poor blood flow in the legs causes fluid buildup, leading to swelling, redness, and dry, peeling skin—usually around the ankles but can spread.
Treatment: Compression socks, leg elevation, moisturizers
Rare but Serious Causes
Some causes of peeling skin are rare but require urgent attention.
Infections That Cause Peeling
- Scarlet fever: “Sandpaper” rash followed by peeling hands and feet
- Staphylococcal scalded skin syndrome (SSSS): Toxin causes skin to slough off
- Kawasaki disease: In children; peeling occurs during recovery phase
Drug Reactions: SJS and TEN
Stevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) are life-threatening reactions to medications (e.g., antibiotics, anticonvulsants).
Warning signs:
– Fever, flu-like symptoms
– Widespread blisters
– Mucosal sores (mouth, eyes)
– Peeling skin in sheets
This is a medical emergency. Seek immediate care.
When to See a Doctor
Most peeling resolves with self-care. But see a healthcare provider if:
Red Flags for Medical Evaluation
- Peeling lasts more than 2–4 weeks
- Signs of infection: pus, warmth, swelling, red streaks
- Open sores, ulcers, or deep cracks
- Spreading beyond the feet
- Pain, burning, or significant discomfort
- History of diabetes or poor circulation
Seek emergency care for:
– Rapidly spreading redness or swelling
– High fever or chills
– Difficulty breathing or swallowing
– Unexplained weight loss or fatigue
Diagnosis: How Doctors Find the Cause

Accurate diagnosis starts with a thorough evaluation.
What to Expect at the Appointment
- Medical history: Medications, allergies, footwear, systemic conditions
- Physical exam: Pattern, symmetry, and location of peeling
- Skin scraping (KOH test): Checks for fungus
- Fungal culture: Confirms diagnosis if KOH is negative
- Patch testing: For suspected allergies
- Skin biopsy: For unusual or persistent cases
- Blood tests: TSH for thyroid, HbA1c for diabetes
Never self-treat if the cause is unclear—wrong treatment can worsen the condition.
Prevention: Daily Habits That Work
Preventing peeling starts with smart foot care.
Essential Foot Hygiene Practices
- Wash daily with mild, fragrance-free soap
- Dry thoroughly, especially between toes
- Moisturize every day with thick, occlusive creams
- Wear breathable shoes (leather, mesh)
- Use cotton or moisture-wicking socks
- Change socks daily (or more if sweaty)
- Rotate shoes to allow 24 hours of drying
- Disinfect shoes with antifungal sprays
Additional Tips
- Wear flip-flops in public showers and pools
- Apply sunscreen to soles when exposed
- Inspect feet daily, especially if diabetic
- Avoid popping blisters or peeling skin manually
Final Note
Peeling skin on the bottom of the feet is usually harmless but can be a sign of something more serious. From dry skin and athlete’s foot to diabetes and autoimmune disorders, the causes vary widely. Most cases improve with proper hygiene, moisturizing, and targeted treatments. However, persistent, painful, or spreading peeling should never be ignored—especially if you have a chronic health condition. Early diagnosis and care prevent complications like infection, ulcers, or long-term skin damage. By understanding the causes and knowing when to seek help, you can keep your feet healthy, comfortable, and protected.