Introduction: Why Does Your First Step Feel Like Walking on Glass?
Imagine waking up, feeling refreshed, and swinging your legs out of bed. But the moment your feet hit the floor, a sharp, stabbing sensation shoots through your heel. You limp to the bathroom, and after a few minutes, the pain dulls into a dull ache—only to return after you’ve been sitting for a while or standing for too long.
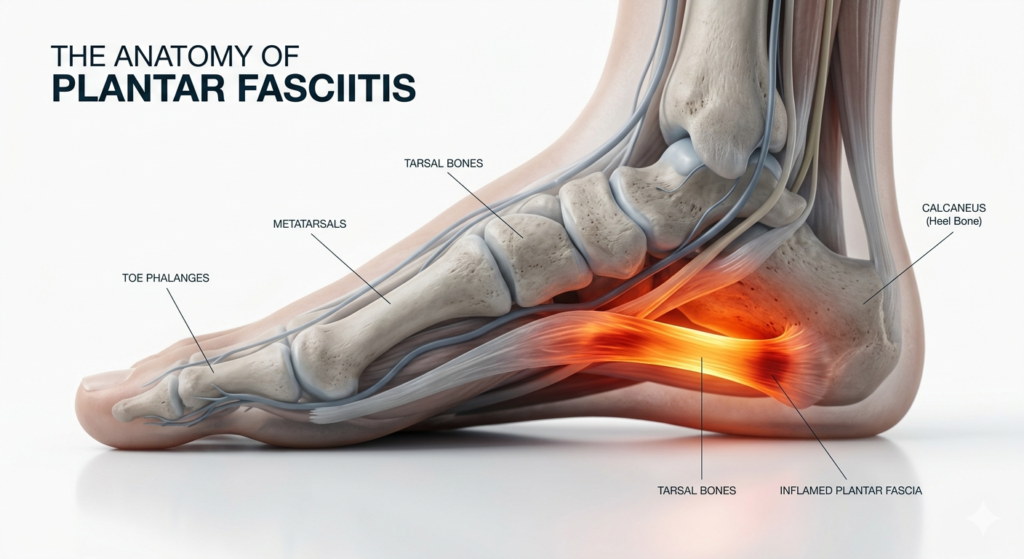
If this sounds familiar, you aren’t alone. You are likely experiencing Plantar Fasciitis, one of the most common orthopedic complaints worldwide. It affects athletes, office workers, and everyone in between. But while the pain is common, it is not something you have to live with.
In this comprehensive guide, we will break down the “what,” “why,” and “how” of this condition. We will explore the biomechanics of your foot, why your current shoes might be your worst enemy, and the exact steps you can take to reclaim your mobility.
1. What is Plantar Fasciitis?
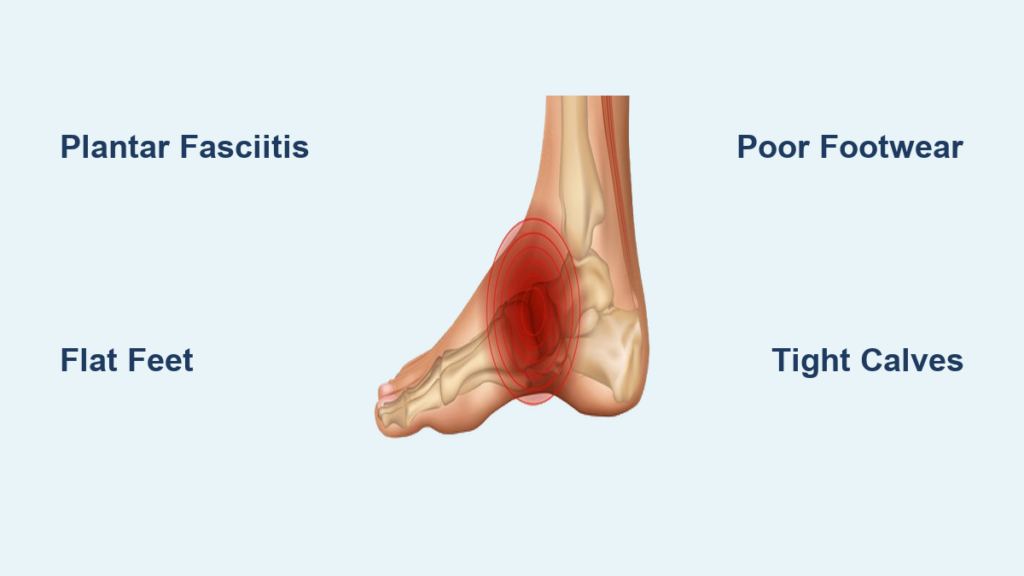
At its core, Plantar Fasciitis is the inflammation of the plantar fascia—a thick, web-like ligament that connects your heel bone to the front of your foot. This ligament acts as a shock absorber and supports the arch of your foot, helping you walk, run, and jump efficiently.
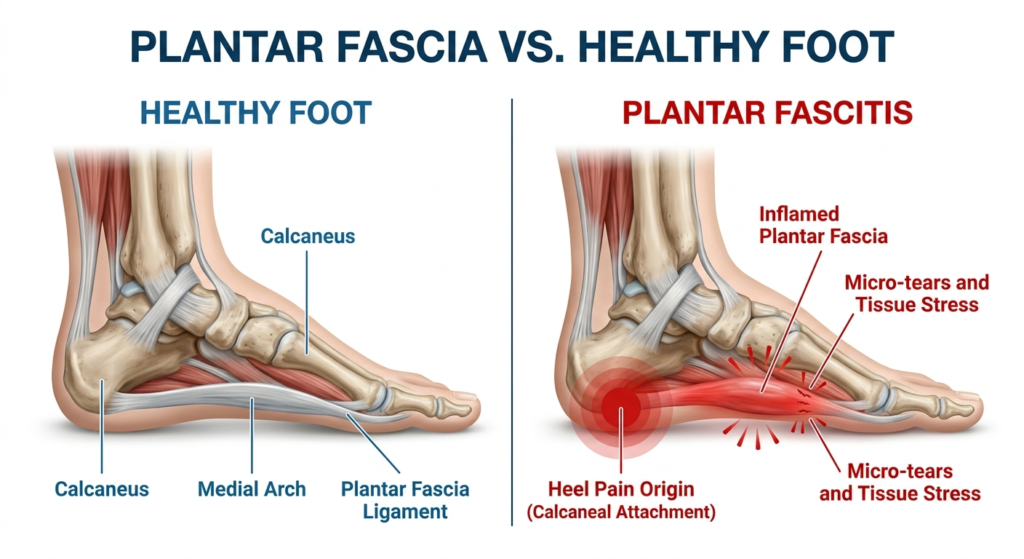
When too much pressure is put on your feet, it can damage or tear the tissues. The body’s natural response to this micro-trauma is inflammation, which results in the hallmark heel pain and stiffness associated with the condition. Unlike a sudden break or sprain, this is typically a “wear and tear” injury that develops over time.
2. How it Works: The Biomechanics of the Arch
Your foot is a masterpiece of engineering. The plantar fascia functions like a bowstring on an archer’s bow. Every time your foot hits the ground, the arch flattens to absorb the impact, stretching the “bowstring.” When you lift your foot, the fascia recoils, helping propel you forward.

When the “bowstring” is stretched too tight or too often, small tears occur. Because the blood supply to ligaments is lower than to muscles, these tears heal slowly. During the night, while you sleep, your foot naturally points downward, allowing the fascia to contract and begin healing in a shortened position. This is why the first step in the morning is so painful—you are essentially re-tearing those healing tissues the moment you put weight on them.
3. Key Benefits of Proper Arch Support and Treatment
Addressing the problem early doesn’t just stop the pain; it prevents a “domino effect” of injuries throughout the body.
- Reduced Inflammation: Proper support allows the ligament to rest and heal without being constantly re-injured.
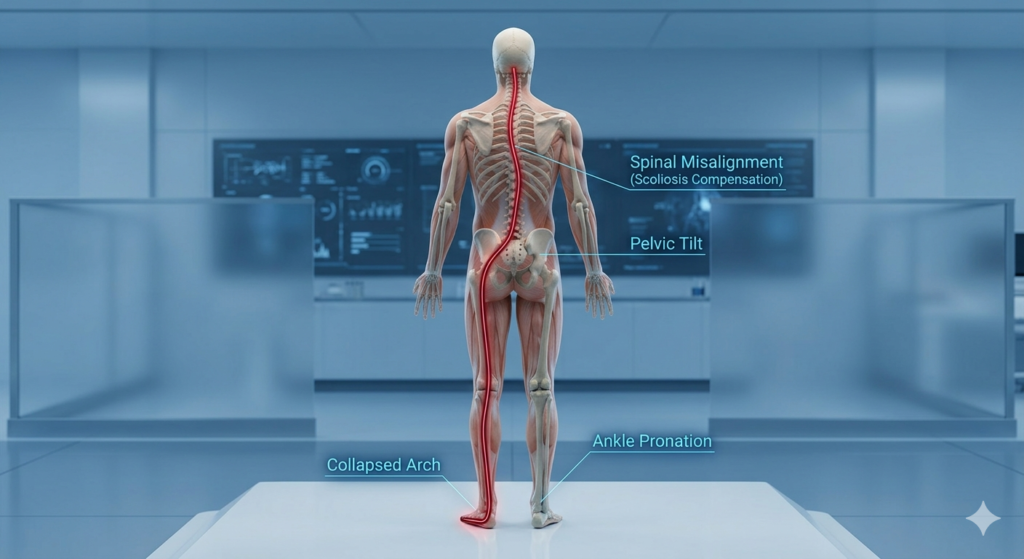
- Correction of Overpronation: Many people’s feet roll inward (overpronate). Arch support keeps the foot in a neutral position.
- Knee and Hip Protection: When your feet are misaligned, your knees and hips compensate, leading to secondary joint pain.
- Enhanced Mobility: Proper treatment allows you to return to the activities you love, from morning jogs to weekend hikes.
4. Common Problems and Mistakes
The biggest mistake most people make is ignoring the pain. They assume it will “go away on its own.” Other common issues include:

- Worn-out Footwear: Running shoes lose their structural integrity after 300–500 miles. Walking in “dead” shoes is a primary cause.
- Sudden Increases in Activity: Moving from a sedentary lifestyle to running a 5K without a ramp-up period.
- Hard Surfaces: Walking barefoot on tile or hardwood floors at home puts maximum stress on the fascia.
- Weight Fluctuations: A sudden increase in weight adds significant pressure to the arches.
5. Step-by-Step Guide to Relieving Foot Pain
If you are currently in pain, follow this recovery protocol:
Step 1: The Frozen Water Bottle Roll
Freeze a plastic water bottle. Sit in a chair and roll your foot over the frozen bottle for 10–15 minutes. This provides both massage (breaking up scar tissue) and cryotherapy (reducing inflammation).
Step 2: Morning Calf Stretches
Before you even get out of bed, use a towel to pull your toes toward your shin. Hold for 30 seconds. This “pre-stretches” the fascia so that first step isn’t as traumatic.
Step 3: Upgrade Your Insoles
Replace the generic foam liners in your shoes with firm, medical-grade arch supports. Look for “orthotics” that do not compress easily under your weight.
Step 4: Avoid Barefoot Walking

Wear supportive slippers or “recovery slides” inside the house at all times.
6. Expert Tips for Long-term Success

- The “Rule of Two”: Never increase your walking or running distance by more than 10% per week.
- Strengthen Your “Foot Core”: Practice picking up marbles with your toes or “scrunching” a towel on the floor to build the intrinsic muscles of the foot.
- Check Your Tread: Look at the bottom of your shoes. If the inside of the heel is worn down more than the outside, you are overpronating and need arch support.
- Night Splints: For chronic cases, wearing a night splint keeps the foot in a neutral position while you sleep, preventing the fascia from tightening.
7. Comparison: Over-the-Counter vs. Custom Orthotics
| Feature | OTC Insoles | Custom Orthotics |
| Cost | $20 – $60 | $300 – $600 |
| Durability | 6 – 12 Months | 3 – 5 Years |
| Accessibility | Immediate (Drugstore) | Requires Podiatrist Visit |
| Best For | Mild to Moderate Pain | Severe Deformities / Chronic Issues |

8. Who is Most at Risk?
You are more likely to develop Plantar Fasciitis if you fall into these categories:

- The Over-40 Club: The fascia loses elasticity as we age.
- Service Workers: Teachers, nurses, and retail workers who spend 8+ hours on hard floors.
- Flat-Footed Individuals: Those with low arches naturally put more strain on the ligament.
- Distance Runners: High-impact repetitive stress is a major trigger.
9. Frequently Asked Questions
Q: Can I keep running with Plantar Fasciitis?
A: It is recommended to switch to low-impact activities like swimming or cycling until the acute pain subsides.
Q: Are flip-flops bad for my feet?
A: Most flip-flops provide zero arch support and force your toes to “grip” the shoe, which worsens the strain. Opt for orthopedic sandals instead.
Q: How long does it take to heal?
A: With consistent treatment, most people feel significant relief in 4–6 weeks, though full healing can take several months.
Q: Does losing weight help?
A: Yes. Your feet carry your entire body weight; even a 5-10 lb reduction can significantly decrease the pressure on your arches.
Q: When should I see a doctor?
A: If the pain persists after a month of home treatment or if you notice redness and swelling, consult a podiatrist.
10. Conclusion: Step Toward a Pain-Free Future

Plantar Fasciitis is a signal from your body that your foundation needs attention. By understanding the mechanics of your foot, investing in proper arch support, and committing to simple daily stretches, you can eliminate the pain and prevent it from ever coming back.
Don’t wait until the pain becomes unbearable. Start with the frozen water bottle roll today, check your shoes for wear, and give your feet the support they deserve.

One thought on “What is Plantar Fasciitis? A Complete Guide to Heel Pain”