Heel pain doesn’t just slow you down—it can stop you in your tracks. If you’ve ever limped to the bathroom first thing in the morning with a sharp, stabbing sensation under your foot, you’re not alone. Plantar fasciitis accounts for up to 80% of heel pain cases, making it the most common culprit. But it’s frequently confused with heel bursitis, a condition that affects the back of the heel and requires a completely different treatment strategy.
Misdiagnosing one for the other can lead to ineffective care, prolonged discomfort, and even worsening symptoms. The key to proper treatment lies in understanding the distinct differences in pain location, timing, response to movement, and visible signs. This guide breaks down every critical sign of heel bursitis vs plantar fasciitis so you can identify what’s really causing your heel pain—and how to treat it effectively.
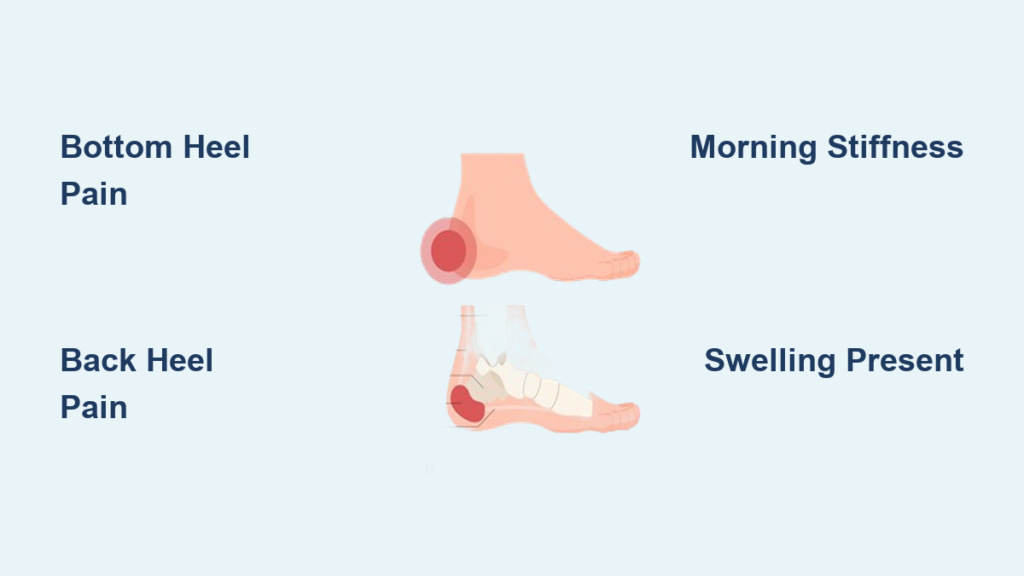
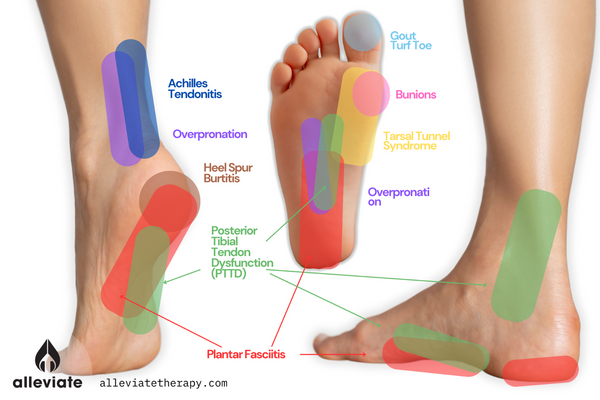
Pain Location: Bottom of Heel vs Back of Heel
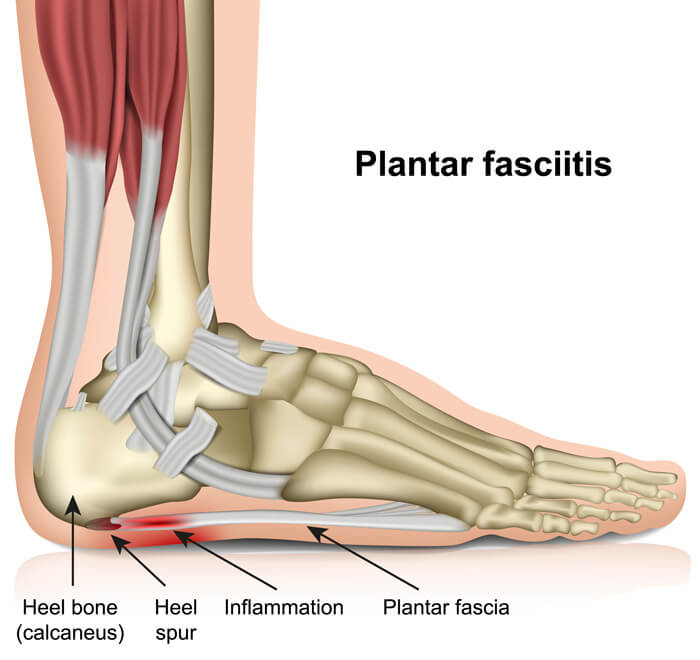
Plantar Fasciitis: Pain Under the Heel
If your pain is on the bottom of the heel, especially toward the inner (medial) side, it’s likely plantar fasciitis. This condition stems from inflammation or degeneration of the plantar fascia, a thick band of tissue that supports the arch and runs from the heel to the toes.
- What to feel for: Press your thumb into the underside of your heel—tenderness at the inner base is a hallmark sign.
- Patient experience: “It feels like stepping on a marble or a piece of glass.”
- Visual clue: The heel looks normal—no swelling or redness—despite intense pain.
Heel Bursitis: Pain Behind the Heel
In contrast, heel bursitis causes pain at the back of the heel, just above the heel bone, near the Achilles tendon. There are two main types:
– Retrocalcaneal bursitis: Inflammation between the Achilles tendon and heel bone.
– Retroachilles bursitis: Inflammation between the skin and Achilles tendon.
- What to feel for: Pain and swelling behind the heel, often worsened by shoe pressure.
- Patient clue: “My shoes rub the back of my heel and make it flare up.”
- Visual clue: A red, swollen bump—commonly called a “pump bump” or Haglund’s deformity.
Clinical Tip: Pain on the bottom? Think plantar fasciitis. Pain on the back that flares with shoe wear? Suspect bursitis.
Pain Patterns: Morning Pain vs All-Day Worsening
Plantar Fasciitis: Worst with First Steps
The classic sign of plantar fasciitis is severe pain with the first steps in the morning or after sitting for a long time. This happens because the plantar fascia tightens overnight, and sudden weight-bearing causes microtearing.
- Pattern:
- 🔹 Sharp pain upon standing after rest
- 🔹 Improves within minutes of walking
- 🔹 Returns after prolonged standing or activity
- Why it happens: Movement warms up the tissue and increases blood flow, temporarily reducing stiffness.
Heel Bursitis: Pain Increases with Use
Heel bursitis follows the opposite pattern: mild or no pain in the morning, but increasing discomfort as the day goes on, especially with walking, running, or wearing shoes.
- Pattern:
- 🔹 Pain-free or mild in the morning
- 🔹 Worsens with activity, especially uphill walking or tiptoeing
- 🔹 Persistent ache by evening
- Why it happens: Repetitive compression and friction on the bursa cause cumulative irritation.
Key Differentiator:
– Pain improves with walking → Plantar fasciitis
– Pain worsens with walking → Heel bursitis
What Makes It Worse? Triggers and Aggravating Factors
Plantar Fasciitis: Pain After Rest and Barefoot Walking
Aggravating Factors
- First steps after sleep or sitting
- Walking barefoot on hard floors
- Prolonged standing (e.g., at work)
- Climbing stairs or hills
- Worn-out or flat shoes with poor arch support
Relief Strategies
- Walking (after initial stiffness)
- Rolling the foot on a frozen water bottle or tennis ball
- Wearing supportive shoes with good arch support
- Using night splints to keep the fascia stretched overnight
Pro Tip: The frozen water bottle roll combines stretching and icing—ideal for reducing both pain and inflammation in plantar fasciitis.
Heel Bursitis: Pain from Shoe Pressure and Activity
Aggravating Factors
- Tight or rigid-heeled shoes (e.g., dress shoes, pumps)
- Uphill walking or running
- Standing on tiptoes
- Direct pressure on the back of the heel
- Aggressive Achilles stretches
Relief Strategies
- Removing shoes or switching to open-back footwear
- Using gel heel pads or heel lifts
- Applying ice to reduce swelling
- Rest and elevation
Warning: If stretching makes your heel pain worse, stop immediately—you may have bursitis or Achilles tendon involvement.
Swelling, Redness, and Visible Signs
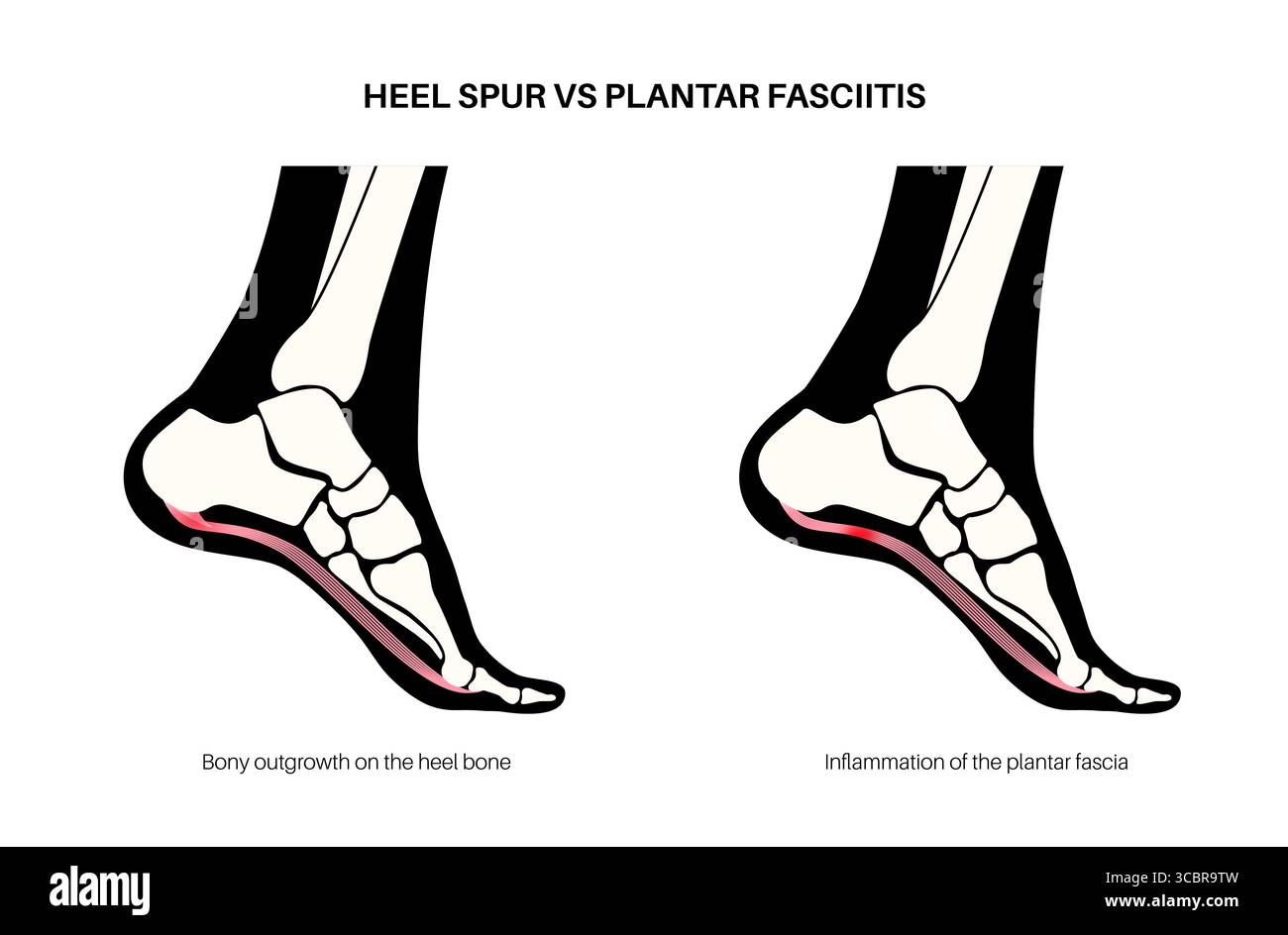
Plantar Fasciitis: No Swelling or Bump
- Swelling: Rare or absent
- Redness or warmth: Not present
- Visible lump: None
The pain is deep and structural, not inflammatory on the surface. The heel appears normal despite significant discomfort.
Heel Bursitis: Swelling, Redness, and “Pump Bump”
- Swelling: Common, especially with retroachilles bursitis
- Redness and warmth: Often present due to active inflammation
- Visible lump: A hard, tender bump may form at the back of the heel—known as Haglund’s deformity or “pump bump”
Clinical Sign: The presence of swelling, redness, or a bump is almost always indicative of bursitis, not plantar fasciitis.
Haglund’s Deformity
- A bony prominence on the upper back of the heel
- Caused by chronic friction from rigid shoes
- Leads to repeated bursa irritation and inflammation
- May require shoe modification or surgery if conservative treatments fail
Response to Stretching and Movement
Plantar Fasciitis: Stretching Helps
Stretching is a core treatment for plantar fasciitis because it reduces tension in the plantar fascia and calf muscles.
Effective Stretches
- Wall calf stretch: 30 seconds, 3–5 times daily
- Towel stretch: Pull toes toward shin while seated
- Foot roll: Use a tennis ball or foam roller under the arch
Why it works: Stretching improves flexibility and reduces strain on the fascia.
Heel Bursitis: Stretching Can Make It Worse
Aggressive stretching—especially of the Achilles tendon—can compress the inflamed bursa, increasing pain.
Movements That Trigger Pain
- Ankle plantarflexion (pointing toes down)
- Standing on tiptoes
- Walking uphill
- Single-leg heel raise: Pain at the back of the heel suggests bursitis or tendonitis
Expert Note: If stretching increases pain, pause and consider bursitis or Achilles tendonitis.
Causes and Risk Factors
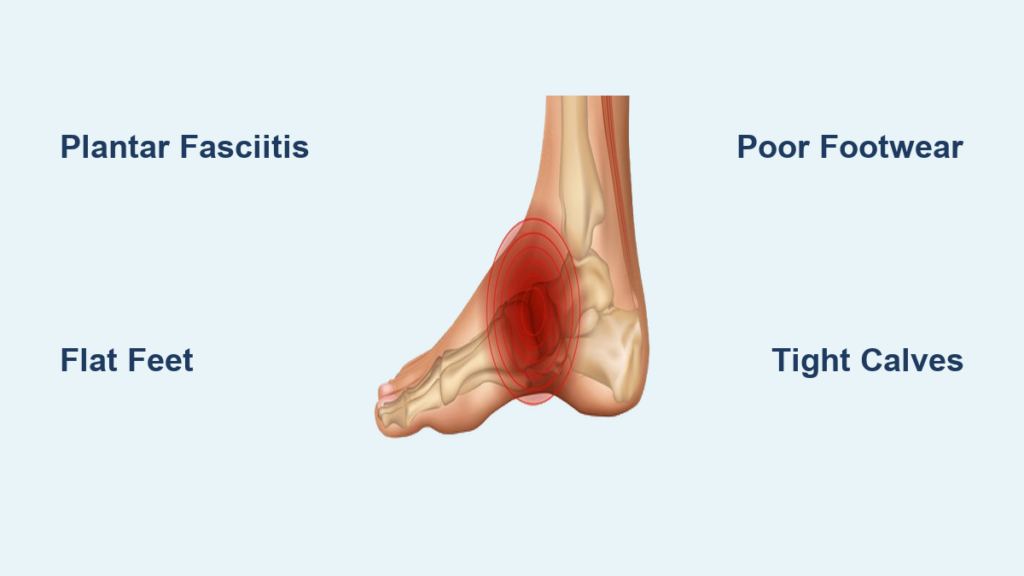
Plantar Fasciitis: Overuse and Biomechanics
Common Causes
- Repetitive strain from running or standing
- Tight calf muscles (limit ankle motion)
- Flat feet or high arches
- Worn-out shoes (loss of cushioning)
- Weight gain or obesity
- Age 40–60 (tissue becomes less elastic)
Occupational Risk
- Jobs requiring long hours on hard floors (teachers, nurses, retail workers)
Fact: Shoes lose support after 6–12 months—replace them to prevent injury.
Heel Bursitis: Friction and Pressure
Retrocalcaneal Bursitis
- Uphill running or jumping
- Tight Achilles tendon
- Haglund’s deformity
- Systemic conditions: Rheumatoid arthritis, gout, psoriatic arthritis
Retroachilles Bursitis
- Shoe friction: Caused by rigid heel counters
- High heels or dress shoes (“pump bump”)
- Flip-flops: Lack heel support, increase rubbing
Note: Both types often occur with Achilles tendonitis due to shared anatomy and stress.
Diagnosis: How It’s Confirmed
Physical Exam: Palpation and Movement Tests
- Plantar fasciitis: Tenderness at medial plantar heel, pain with passive toe extension
- Heel bursitis: Tenderness above the heel bone, swelling, pain with ankle plantarflexion
- Tinel’s sign: Tingling when tapping the posterior tibial nerve—helps rule out tarsal tunnel syndrome
Imaging: Ultrasound, X-ray, MRI
| Test | What It Shows |
|---|---|
| Ultrasound | Thickened plantar fascia (>4 mm), fluid in bursae |
| X-ray | Heel spurs, Haglund’s deformity, fractures |
| MRI | Gold standard—differentiates fasciitis, bursitis, tendonitis, nerve issues |
Expert Advice: If pain lasts more than 2–3 weeks, get imaging to avoid misdiagnosis.
Treatment: Condition-Specific Care
Plantar Fasciitis: Stretch, Support, Stabilize
- Rest, ice, NSAIDs
- Stretching, night splints, orthotics
- Shockwave therapy or steroid injections if chronic
Heel Bursitis: Rest, Modify, Protect
- Rest, ice, NSAIDs
- Shoe changes, heel pads, heel lifts
- Ultrasound-guided steroid injections, physical therapy, or surgery if severe
Warning: Repeated steroid injections can weaken tendons—use sparingly.
When to See a Doctor
Seek help if:
– Pain lasts more than 2–3 weeks
– You have swelling, redness, or fever (possible infection)
– Can’t bear weight (fracture or rupture)
– Numbness or tingling (nerve issue)
Best Specialist: A podiatrist or foot and ankle orthopedist.
Key Differences at a Glance
| Feature | Plantar Fasciitis | Heel Bursitis |
|---|---|---|
| Pain Location | Bottom of heel | Back of heel |
| Pain Timing | Worst in morning | Worse with activity |
| Swelling | No | Yes, often visible |
| Shoe Pain | Not typical | Aggravated by heel counter |
| Stretching | Helps | May worsen |
| Redness/Warmth | No | Yes, common |
| Imaging Sign | Fascia >4 mm thick | Fluid-filled bursa |
| Main Treatment | Stretching, orthotics | Rest, shoe changes, heel lifts |
Final Note
Accurate diagnosis is critical. Treating bursitis like plantar fasciitis—especially with aggressive stretching—can delay healing and increase pain. Conversely, ignoring arch support in plantar fasciitis leads to chronic issues.
If your heel pain isn’t improving, don’t guess—get evaluated. With the right diagnosis, most cases resolve within weeks using targeted, conservative care. Whether it’s the bottom or back of your heel, understanding the signs of heel bursitis vs plantar fasciitis puts you on the fast track to relief.